
Getting the wrong diagnosis code on a BCBS claim can be a frustrating and costly mistake. This is often caused by incorrect coding by the healthcare provider, which can lead to denied claims and delayed payments.
Incorrect coding can occur when the provider doesn't accurately document the patient's condition or when the coder doesn't properly assign the correct codes from the ICD-10 manual. According to the article, the most common incorrect codes used by healthcare providers are those related to chronic conditions, such as diabetes and hypertension.
To prevent this issue, healthcare providers can take steps to ensure accurate coding. This includes verifying the patient's medical record and using the correct ICD-10 codes for each diagnosis.
For your interest: Bcbs Advocate Hmo Providers
Understanding Medical Claims
Medical claims are submitted by healthcare providers to insurance companies like BCBS for payment. These claims must contain specific information, including patient details, procedure codes, and most importantly, diagnosis codes.
Diagnosis codes explain the medical condition being treated and justify the services or procedures billed. If these codes are inaccurate or invalid, claims are often denied, delayed, or flagged for further review.
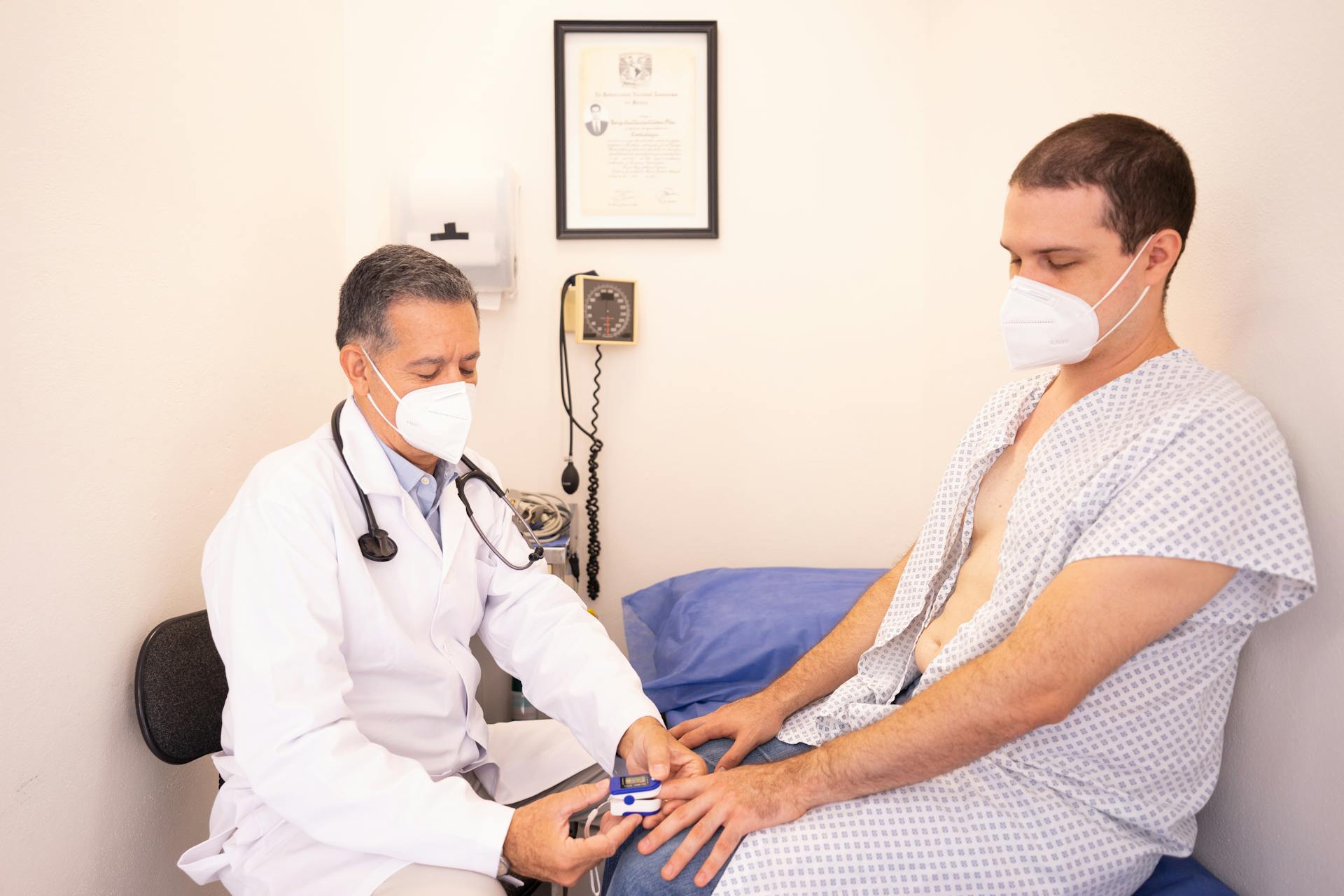
Accurate diagnosis coding is critical in medical billing, ensuring that healthcare providers are paid appropriately and that patients are billed for the correct services. Incorrect or invalid diagnosis codes can result in claim denials.
Diagnosis codes, particularly ICD (International Classification of Diseases) codes, are critical in medical billing. They allow BCBS and other insurers to understand the medical condition that is being treated.
Medical billing software is a crucial tool in preventing invalid diagnosis codes from being submitted to BCBS. Features such as real-time code validation, auto-updating code libraries, and claim scrubbing tools can help prevent errors.
Here are some key features of medical billing software that can help prevent invalid diagnosis codes:
- Real-Time Code Validation: Software can alert users to outdated or incorrect codes before submission.
- Auto-Updating Code Libraries: Ensure that the software is updated with the latest ICD codes automatically.
- Claim Scrubbing: Claim scrubbing tools check for common errors and discrepancies, reducing the chances of rejections.
Common Causes and Solutions
Typing errors can be a common cause of invalid diagnosis codes on BCBS claims. A single misplaced digit or incorrect letter can lead to a code being flagged as invalid.
Code mismatch is another issue that can cause problems. If the diagnosis code doesn't match the treatment or procedure performed, it can cause confusion and lead to an invalid code.
Expired codes can also be a problem. The ICD system is updated regularly, and codes that were once valid may no longer be accepted.
System issues can also cause errors. Software glitches or improper system updates can lead to invalid codes being generated.
Provider or payer errors can also lead to wrong or outdated codes being used. Miscommunication between healthcare providers and BCBS can cause problems.
Here are some common causes of invalid diagnosis codes on BCBS claims:
Appealing and Preventing Issues
If your BCBS claim is denied due to an invalid diagnosis code, you can take steps to appeal the decision. Gather all relevant documentation, including patient records, the original claim, and any correspondence from BCBS.
To appeal a denied claim, you'll need to fill out an appeal form provided by BCBS, ensuring all required fields are completed. This form is a crucial step in the appeal process.
When submitting an appeal, make sure to attach supporting documents that justify the diagnosis and treatment, as well as a corrected claim. This will help strengthen your case and increase the chances of a successful appeal.
Suggestion: Bcbs Clinical Appeal Form

After submitting the appeal, follow up with BCBS to ensure it is being processed. This will help you stay on top of the situation and ensure that your appeal is not lost in the shuffle.
To avoid recurring diagnosis code errors, it's essential to double-check codes before submission. This means verifying that the codes used are accurate and up-to-date.
Having a second person review claims for accuracy before submission can also help prevent errors. This can be a colleague, a supervisor, or even a coding expert.
Here are some steps to implement a review process:
- Assign a second person to review claims for accuracy.
- Provide them with access to online coding resources or printed ICD-10 guides.
- Establish a checklist to ensure all necessary codes are included.
By following these steps, you can reduce the risk of diagnosis code errors and ensure that your BCBS claims are processed correctly.
Accurate Coding and Resources
Accurate coding is crucial for successful BCBS claims. Regularly updating your ICD code list is essential, as the ICD system is frequently updated.
You can use code validation tools to catch potential coding issues before submission. Many billing platforms have built-in validation tools that can help reduce errors.
To stay up-to-date, consider the following resources:
- The Centers for Medicare & Medicaid Services (CMS) provides updates on ICD-10 codes and guidelines.
- The American Medical Association (AMA) offers training and resources for medical coders.
- Coding books or online subscriptions can be updated annually to keep your ICD-10 coding knowledge current.
Core Importance of Medical Standards

Accurate diagnosis coding is crucial for healthcare providers to get paid appropriately. Accurate diagnosis coding ensures that patients are billed for the correct services.
Incorrect or invalid diagnosis codes can result in claim denials, impacting revenue flow and patient care continuity. This can be a major problem for healthcare providers.
Diagnosis codes, particularly ICD (International Classification of Diseases) codes, are critical in medical billing. They allow insurers to understand the medical condition being treated.
Accurate diagnosis coding is not just about getting paid, it's also about providing good patient care.
Curious to learn more? Check out: Patient Advocate Insurance
Ways to Mitigate DoS
To mitigate Denial of Service (DoS) attacks, you can implement various strategies. Double-checking claim information is crucial to prevent errors or omissions that may lead to denials.
Utilizing electronic claim submission is another effective way to reduce the chances of errors or omissions. Electronic claim submission systems often have built-in validation checks that can flag missing or incorrect information before the claim is submitted.
Check this out: Medical Information Bureau Mib

Implementing claim scrubbing software can automatically review claims for errors or missing information. This software can help identify any issues before the claim is submitted, allowing for corrections to be made in a timely manner.
Conducting regular staff training is essential to ensure that your billing and coding staff are up-to-date with the latest coding guidelines and requirements. This can help reduce the likelihood of errors or omissions that may lead to denials.
Establishing clear communication channels between your billing and coding staff, providers, and payers is also vital. This can help ensure that all parties are aware of any specific requirements or documentation needed to support the claim and prevent denials.
Here are some key strategies to mitigate DoS attacks:
- Double-check claim information
- Utilize electronic claim submission
- Implement claim scrubbing software
- Conduct regular staff training
- Establish clear communication channels
Accurate Coding with ICD-10
Accurate Coding with ICD-10 is crucial for submitting claims to BCBS. Regularly updating your ICD code list is essential, as the ICD system is frequently updated.
You should ensure your software and staff are using the most recent codes. This will help prevent errors and ensure accurate coding.
Expand your knowledge: Enjoy Coding

Training your billing staff on ICD-10 coding is also vital. Ongoing education can help reduce the risk of errors and improve coding accuracy.
Using code validation tools can catch potential coding issues before submission. Many billing platforms have built-in validation tools that can help streamline the coding process.
Here are some key points to keep in mind:
- Regularly update your ICD code list
- Train your billing staff on ICD-10 coding
- Use code validation tools
Accurate Coding Resources
Accurate Coding Resources are crucial for healthcare providers to ensure their claims are processed smoothly. Regularly updating your ICD code list is essential, as the ICD system is frequently updated.
You can find the most recent codes on the Centers for Medicare & Medicaid Services (CMS) website. The CMS provides updates on ICD-10 codes and guidelines, which is a valuable resource for accurate coding.
Training your billing staff on ICD-10 coding is also vital, as ongoing education can help reduce the risk of errors. Many billing platforms have built-in validation tools that can catch potential coding issues before submission.
Here are some additional resources to keep in mind:
Accurate diagnosis coding requires ongoing effort and attention to detail. By staying informed and using the right resources, you can reduce the risk of errors and ensure your claims are processed smoothly.
Coding Advice
If you receive a remark code M63 on the remittance advice, it means there is an invalid diagnosis code or the diagnosis code submitted on the claim is not permitted as the primary diagnosis code. This can result in claim denials and impact revenue flow.
To correct this issue, submit a corrected claim and/or an adjustment form using the button below. If you're submitting this form by mail, please send it to PO Box 2266 in Cheyenne, WY 82003, or by fax at (307) 432-2942.
CAT II codes are used for diagnostic/screening processes or results, and it's essential to use the correct codes to avoid claim denials.

Here are some common reason codes and remark codes to be aware of:
Remember, accurate diagnosis coding is crucial for reimbursement review, and medical coders play a vital role in ensuring claims are accurate.
Denial and Resolution
If your BCBS claim is denied due to an invalid diagnosis code, don't worry - it's not the end of the road. You can appeal the decision by gathering documentation, including patient records and original claim details.
To appeal a denied claim, you'll need to fill out an appeal form provided by BCBS, ensuring all required fields are completed. This will help you get your claim back on track.
If your claim is denied due to Denial Code 12, it means the diagnosis doesn't match the provider type. You can check the 835 Healthcare Policy Identification Segment for more details.
To help you navigate the appeal process, here's a quick checklist:
- Gather all relevant documentation
- Fill out the appeal form and attach supporting documents
- Follow up with BCBS to ensure your appeal is being processed
Remember to stay on top of your appeal and follow up with BCBS to ensure it's being processed.
Denial 12

Denial 12 means the diagnosis doesn't match the provider type. This can be a frustrating experience, especially if you're confident that your diagnosis is correct.
To resolve Denial 12, you'll need to review the 835 Healthcare Policy Identification Segment for more details. This segment provides important information about the claim, including the provider type and the diagnosis.
One common cause of Denial 12 is a mismatch between the provider type and the diagnosis code. For example, if you're a primary care physician billing for a surgical procedure, your diagnosis code may not match the provider type.
Here are some steps you can take to resolve Denial 12:
- Review the claim thoroughly to ensure that all related or qualifying claim/services are accurately identified and included.
- Double-check the documentation and coding to verify that the related claim/service was properly documented and coded.
- Check the 835 Healthcare Policy Identification Segment for more details on the provider type and diagnosis code.
- If necessary, update the diagnosis code or provider type to ensure that they match.
- Resubmit the claim through the appropriate electronic submission channel.
By following these steps, you can resolve Denial 12 and get your claim processed correctly.
Denial 146
Denial 146 is a common issue that can be frustrating to deal with. It means the diagnosis reported for the service date(s) was not valid.
This denial code is often used when the insurance company receives a claim with a diagnosis that doesn't match the medical services provided. Denial code 146 is a clear indication that something is off.
To resolve a denial code 146, you'll need to review the claim and verify the diagnosis reported. This may involve contacting the healthcare provider or requesting additional documentation.
A valid diagnosis is essential to getting your claim approved, so make sure to double-check the information.
Take a look at this: Bcbs Denial Codes List
Medical Billing and Validation
Medical billing and validation are crucial steps in ensuring that BCBS claims are accurate and submitted correctly. Medical claims are submitted by healthcare providers to insurance companies like BCBS for payment.
Consider reading: Claims for Bcbs Are Submitted to the

To prevent invalid diagnosis codes from being submitted, medical billing software is a vital tool. Features such as real-time code validation, auto-updating code libraries, and claim scrubbing tools check for common errors and discrepancies, reducing the chances of rejections.
Medical coders play a vital role in ensuring claims are accurate. Certified coders are trained to use ICD-10 codes correctly and communicate with providers to ensure the documentation supports the chosen diagnosis codes.
Accurate diagnosis coding ensures that healthcare providers are paid appropriately and that patients are billed for the correct services. Incorrect or invalid diagnosis codes can result in claim denials, which impact revenue flow and patient care continuity.
Here are some key features of medical billing software that can help prevent invalid diagnosis codes:
- Real-Time Code Validation: Software can alert users to outdated or incorrect codes before submission.
- Auto-Updating Code Libraries: Ensure that the software is updated with the latest ICD codes automatically.
- Claim Scrubbing: Claim scrubbing tools check for common errors and discrepancies, reducing the chances of rejections.
By using medical billing software and having certified medical coders, healthcare providers can reduce the risk of claim denials and ensure accurate payment for services rendered.
Specific Diagnoses and Codes

To avoid getting wrong diagnosis codes invalid on BCBS claims, it's essential to regularly update your ICD code list. This means ensuring your software and staff are using the most recent codes, as the ICD system is frequently updated.
You can use code validation tools, which many billing platforms have built-in, to catch potential coding issues before submission. This can help reduce the risk of errors.
Training your billing staff with ongoing education on ICD-10 coding is also crucial. This can help them stay up-to-date on the latest coding guidelines and avoid common mistakes.
To get started, consider the following steps:
- Regularly update your ICD code list.
- Train your billing staff on ICD-10 coding.
- Use code validation tools to catch potential coding issues.
Frequently Asked Questions
What is the denial code for invalid diagnosis?
The denial code for invalid diagnosis is M76. This code indicates a claim rejection due to missing, incomplete, or invalid diagnosis information.
What is the denial code for diagnosis inconsistent with procedure?
Denial code 11 indicates a mismatch between the diagnosis and procedure, requiring further review
Sources
- https://emdeonmdllc.com/bcbs-claim-getting-wrong-diagnosis-code/
- https://med.noridianmedicare.com/web/jadme/topics/ra/denial-resolution/m76-16
- https://www.bcbswy.com/section/providers/page/3/
- https://telehealth.hhs.gov/providers/billing-and-reimbursement/billing-and-coding-medicare-fee-for-service-claims
- https://www.mdclarity.com/denial-code/107
Featured Images: pexels.com

